Next Generation
PhD Health Data Scientists
We train health data scientists, computer scientists, software developers, and AI and machine learning researchers to become research and innovation leaders
Our ambition
The EPSRC Centre for Doctoral Training in Data-Driven Health (DRIVE-Health) trains the next generation of health data scientists, computer scientists, software developers, and AI and machine learning researchers - a crucial component in the drive towards sustainable, equitable global healthcare.
Co-created with the NHS, patients, health tech and pharma, our interdisciplinary PhD training programme is delivered within an active NHS environment and focuses on optimising informatics technologies to address complex global healthcare challenges. By combining academic rigour with real-world applications, the EPSRC DRIVE-Health bridges the gap between complex healthcare needs and technological advancements.
To provide world-class training in health data science research to the next generation of health data scientists, who will have the multidisciplinary skills needed to enable transformations in public health and breakthrough treatments

To solve the most challenging problems in data-driven health research, through a diverse community of the brightest minds in health data science; and an open, collaborative culture which fosters exchange and innovation
To co-create a translational cross-sector collaboration with the NHS, industry, enterprise, policy makers and academia - a first of it's kind for health informatics training in the UK. We work with our broad network of strategic partners to ensure that the UK health sciences sector remains at the global forefront of innovation
Our science and learning environment
There are significant opportunities to revolutionise the delivery of healthcare, with the growing availability of biological, social, genomic, imaging and sensor/Internet-of-Things datasets and electronic health records.
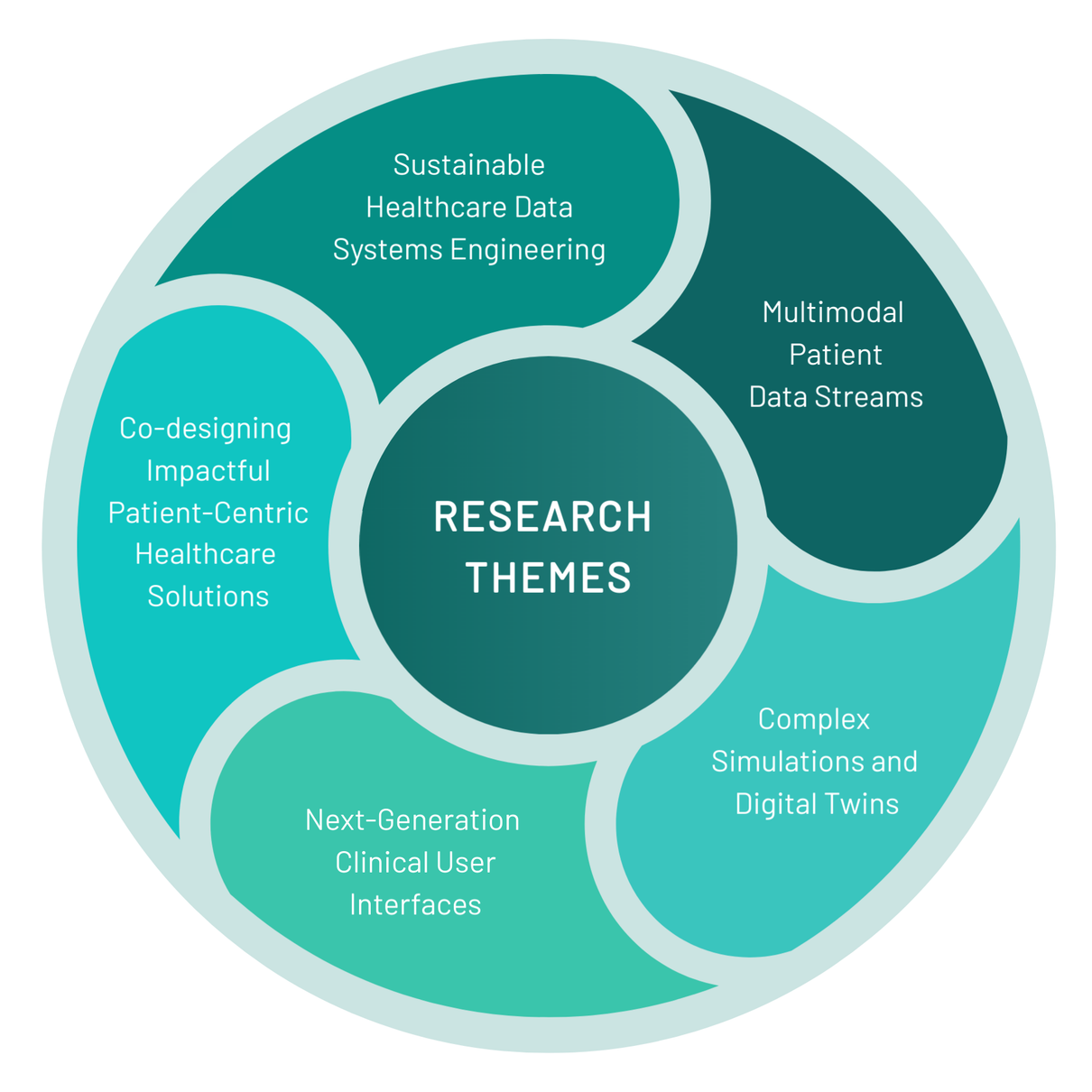
DRIVE-Health PhD programmes focus on 5 key scientific research themes.
News, Views & Insights